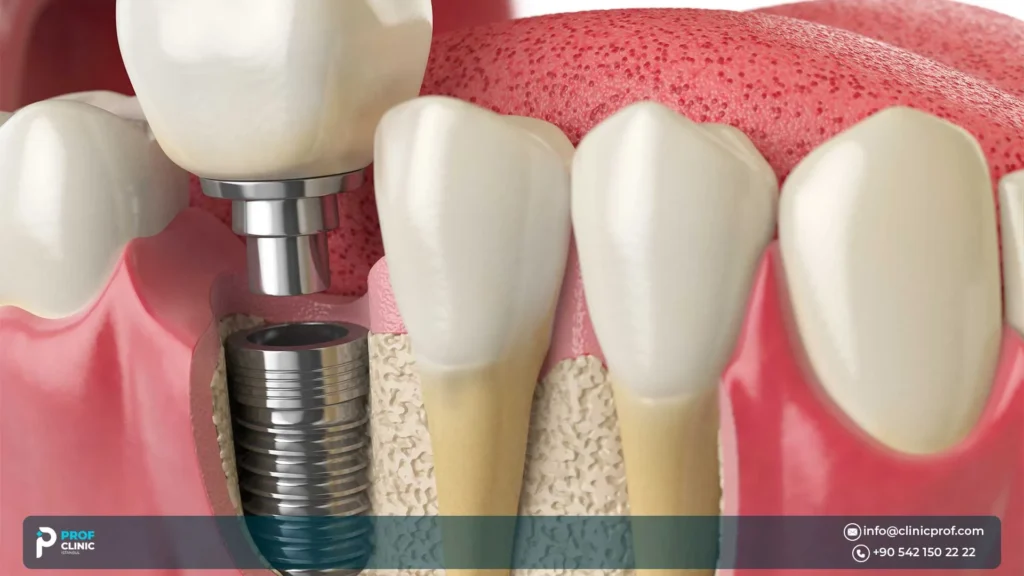
If you’re researching lower jaw all on 4, you’re probably not looking for hype. You want a mandibular-specific explanation: how it works in the bottom jaw, what happens on surgery day, whether “fixed teeth fast” is realistic, and what results actually feel like when you chew, speak, and live normally again.
For patients considering lower jaw All-on-4 in Turkey, the key questions are usually nerve safety, immediate loading, and how stable fixed teeth will feel after healing.
This article by Prof Clinic Istanbul is educational and can’t diagnose you. A qualified dentist must confirm candidacy after an exam, CBCT imaging, and medical history review.
What is Lower Jaw All-on-4?
Mandibular all on is a full-arch implant solution where four dental implants support a fixed bridge that replaces an entire lower set of teeth. It’s not “one implant per tooth.” It’s a strategic, full-arch design aimed at giving you stable bottom teeth implants function with fewer implant sites.
The bottom teeth implants is commonly considered when you have:
- Complete lower-tooth loss (edentulous lower jaw)
- Many failing lower teeth (infection, mobility, repeated fractures) where saving teeth is no longer predictable
- A lower denture that slips, hurts, or makes chewing difficult
What does lower jaw All-on-4 replace?
- The entire lower arch of teeth with one fixed bridge (anchored on implants)
- Often replaces the need for a removable lower denture (case-dependent)
“Fixed teeth” often means a fixed temporary bridge first, with the final bridge placed later after healing and bite refinement, especially if immediate loading is planned.
For broader context without repeating everything here, you can also read our full guide: All-on-4 Dental Implants in Turkey.
Also read: Same-Day All-on-4: Teeth in One Day Possible?
How the Lower Jaw All-on-4 Procedure Works in Istanbul?
A mandibular all on 4 plan starts with one goal: place implants safely and prosthetically, meaning the implants aren’t just “in bone,” but positioned to support a strong, hygienic, well-fitting fixed bridge.
What planning usually includes
- Clinical exam + gum health check: active infection or uncontrolled periodontal disease must be addressed first.
- Bite evaluation: your dentist checks how your jaws meet, any bite collapse, and whether grinding/clenching is likely.
- CBCT (3D imaging): confirms bone volume and maps critical anatomy. especially the inferior alveolar nerve and the mental foramen/mental nerve region in the lower jaw.
- Medical review: conditions like uncontrolled diabetes, bleeding risks, or certain medications may require medical clearance or modified planning.
Why the nerve discussion matters?
In the mandible, the nerve that supplies feeling to the lip and chin travels inside the jawbone and exits near the premolar region (mental foramen). Some people also have an “anterior loop” variation—one reason CBCT is used to reduce nerve-related risk.
Depending on your case, the plan may also include:
- Extractions (if failing teeth remain)
- Bone smoothing/reshaping (alveoloplasty) to create a stable foundation for the bridge and hygiene space
- A choice between immediate loading (fixed temporary soon after surgery) vs delayed loading (bridge later)
What Happens During Lower Jaw All-on-4 Surgery in Istanbul?
For patients traveling to Istanbul for lower jaw All-on-4 treatment, surgery-day planning usually includes imaging review, anesthesia preparation, implant placement, and a written recovery plan before travel home.
Pre-op and anesthesia options
Most lower jaw All-on-4 surgeries are done with local anesthesia. Some patients may also have sedation depending on the clinic’s protocol, medical history, and anxiety level.
Before surgery, your team may review:
- Medications (especially blood thinners—never stop them on your own)
- Recent labs or medical clearance if needed
- A tailored post-op plan (pain control and antibiotics only when prescribed)
The goal is not “zero discomfort.” The goal is safe, controlled surgery and a clear recovery plan.
Implant placement & why the back implants are angled?
All-on-4 is classically described as:
- Two straight anterior implants in the front of the jaw
- Two posterior implants placed at an angle, commonly up to around 45°, depending on anatomy and prosthetic design
Why angle the posterior implants in the lower jaw?
Because it can help your clinician:
- Use available bone in a favorable area
- Reduce how far the bridge “hangs back”
- Work around anatomical limits, especially the mandibular nerve pathway and the mental foramen zone, which must be respected with CBCT planning
Many protocols focus on the interforaminal region, between the mental foramina, for safety and bone availability, then the prosthesis design and implant angulation help support the back teeth region.
If you want to compare this with other full-arch options (without losing the lower-jaw focus), see: Full Arch Dental Implants.
Visit our dental implants page to learn more about our services
Immediate Loading for Lower Jaw All-on-4 in Turkey
“Teeth in a day” can be real, but the most important word is temporary.
What does immediate loading actually mean?
Immediate loading means a fixed temporary bridge may be attached soon after implant placement if stability criteria are met (your team checks this during surgery).
Why are final teeth placed later?
Even when you leave with fixed temporary teeth, the final bridge usually comes later because your team needs time for:
- Bone integration (osseointegration) and soft-tissue healing.
- Bite refinement, especially important in the mandible with high bite forces.
- Final material selection and long-term fit.
If stability isn’t sufficient on surgery day, your dentist may switch to a safer plan. That’s not failure; that’s risk control.
For a deeper breakdown that we, at Prof Clinic in Turkey, use consistently, see: Same Day All-on-4 (Temporary vs Final Teeth & Timeline).
If you’re traveling to Istanbul, Turkey for treatment, schedule a meeting and ask for a written plan that states whether immediate loading is likely and what happens if you’re not a candidate on surgery day.
Results you can expect from bottom teeth implants
When people ask about “lower jaw All-on-4 results,” they usually mean: Will it feel stable? Can I chew? Will it look natural?
Function and chewing
Compared with a loose lower denture, a fixed bridge on implants often feels more stable for chewing and daily comfort, especially once healing progresses and the bite is properly adjusted.
Bite comfort and jaw function
The mandible experiences strong forces and complex movement. That means your result depends on:
- A stable implant foundation
- A prosthesis designed for your bite, not just pretty teeth
- Managing overload, especially if you grind or clench
If you have significant bite collapse, jaw-joint symptoms, or severe wear, your case may require staged planning rather than assuming All-on-4 alone “fixes everything.”
Speech and adaptation
Speech often improves when a slipping denture is replaced, but you may still need an adaptation period while your tongue and muscles adjust to a new fixed bridge shape.
The maintenance reality
A fixed bridge still needs daily care. You’ll likely clean:
- Under the bridge (special floss/threaders or water flosser)
- Around implant sites
- With professional maintenance at intervals your dentist recommends
If you want visuals to understand possibilities with the right mindset that results vary, our Before & After gallery can help set expectations.
Benefits and candidacy for mandibular all on
Key benefits of All-on-4 for the lower jaw
Potential benefits
- Fewer implant sites than some traditional full-arch designs
- A pathway to fixed bottom teeth implants rather than a removable denture
- May reduce the need for extensive grafting in many cases because angled posterior implants can use available bone and avoid certain anatomical limits
Evidence
Always read this with context, not as a guarantee. A systematic review reported very high short-term survival (>24 months) around 99.8% across included studies, but also noted evidence limitations (study quality, follow-up length, and attrition).
In real life, outcomes depend heavily on case selection, habits, and maintenance.
Who is a good candidate
Common good fit patterns include:
- You have a fully missing lower arch, or many failing teeth with a plan for extraction
- You can commit to hygiene and follow-up
- CBCT shows adequate bone in key zones for safe placement and stability
Bone loss in the lower jaw
All-on-4 is often used in atrophic jaws to avoid more invasive grafting routes, but the decision is imaging-driven—not a blanket “graftless” promise.
To answer the question: “Am I a candidate for lower jaw All-on-4?”, use this chechklist
You’re more likely to be suitable if most of these are true:
- I’m missing most/all lower teeth, or they’re clearly failing
- My gum disease is treated/controlled, or I’m willing to treat it first
- I can attend follow-ups and maintain daily cleaning
- I don’t smoke, or I’m willing to reduce or stop, especially during healing
- I don’t have uncontrolled diabetes or unmanaged medical issues
- I don’t grind heavily, or I’m open to protective strategies
The only honest way to confirm mandibular All-on-4 eligibility is CBCT and bite evaluation. Book an appointment and ask for a written rationale for the design chosen (All-on-4 vs more implants)
If you’re comparing “4 vs more implants,” this guide helps without derailing: All-on-4 vs All-on-6.
Also read: Same-Day All-on-4: Teeth in One Day Possible?
Lower Jaw vs Upper Jaw All-on-4 in Turkey
Our patients often ask us if the lower jaw is more stable than the upper. The real answer is: it can be, but the constraint types are different.
Key anatomical differences
- Upper jaw: Often softer bone; sinus anatomy may limit posterior placement
- Lower jaw: Denser bone in many patients, but critical nerve anatomy must be protected; bite forces are typically higher
Some research reports higher implant stability measures in the mandible compared with the maxilla, while also showing stability changes over the first months of healing. Still, your individual result depends on your bone type, surgical technique, and loading protocol.
Practical takeaway:
- Lower jaw cases may feel solid earlier for some patients
- But force management (bite adjustments, avoiding overload, and sometimes a night guard) can be especially important
If you’re comparing arches, we have a dedicated guide on the upper arch: Upper Jaw All-on-4.
All-on-4 vs traditional dental implants
Traditional implants can mean different things:
- Many implants supporting a full-arch bridge
- A different full-arch distribution design
- In some contexts, individual implants and crowns, less common for a fully edentulous arch
Here’s a mandibular-focused decision table to clarify tradeoffs without talking prices:
| Decision factor | Lower Jaw All-on-4 | Traditional full-arch implant approach |
| Primary goal | Fixed full-arch bridge supported by 4 implants | Fixed full-arch solution with more implant sites or different staging |
| Typical implant count | 4 | Often more (case-dependent) |
| Treatment pacing | Can be designed for immediate loading in selected cases | May be staged more often (depends on stability, bone, and plan) |
| Bone graft likelihood | May reduce grafting needs in many anatomies, CBCT decides | May include grafting or alternative designs depending on bone and goals |
| “Teeth in a day” potential | Often possible as fixed temporary if stability criteria are met | Sometimes possible; other times delayed for risk control |
| Hygiene complexity | Daily cleaning under a full-arch bridge is required | Similar, but design details affect access and maintenance |
| Typical best use-case | Full lower arch replacement with strategic implant distribution and controlled bite forces | Patients needing more support distribution, complex bite demands, or specific anatomical constraints |
If you want to explore broader designs and decision drivers, see: Full Arch Dental Implants and All-on-4 vs All-on-6.
Risks and complications of bottom teeth implants
Any surgery has risks. Talking about them clearly is part of safe care, not negativity.
Possible complications
- Infection or delayed healing
- Failure of integration: One implant doesn’t integrate as expected
- Prosthesis issues: Loosening, fracture, chipping, wear
- Bite overload: Especially in strong lower jaws and bruxism
- Gum inflammation around implants
What protects your result
- CBCT-based planning and clear surgical-prosthetic coordination
- Smoking reduction, especially around surgery and healing
- Daily cleaning under the bridge and professional maintenance
- Bite management
- Keeping follow-up appointments, even after you travel home
If you need help coordinating your evaluation or follow-up plan, use Contact us or book an appointment. Also, for our team accountability and credentials, see our Medical Team page.
Lower jaw all on 4 can be a strong solution for people who want stable, fixed bottom teeth implants function, especially when a lower denture is failing or lower teeth can’t be saved predictably. The best results come from mandibular-specific planning: CBCT nerve mapping, bite evaluation, and an honest discussion about whether you qualify for immediate loading or a safer staged timeline.
Talk to our medical team about your CBCT findings, bite forces, and realistic material/timeline options, and ask for a written plan that labels temporary vs final teeth clearly.
FAQs about lower jaw all on 4
How long does the All-on-4 procedure take for the lower jaw?
It depends on whether extractions are needed, your bone condition, and whether you’re receiving a fixed temporary bridge the same day. The most accurate estimate comes after an exam and CBCT planning.
Is the All-on-4 lower jaw procedure painful?
Local anesthesia is commonly used, and some patients may have sedation depending on medical factors and clinic protocol. After surgery, discomfort is expected, and pain control should be guided by your dental team.
What is the recovery time after lower jaw All-on-4 surgery?
Early healing is usually days to weeks, while deeper integration takes longer. If you have immediate loading, protecting the temporary bridge with diet and bite-force limits can matter a lot. Final timing varies by protocol and healing response.
What are the risks or complications of lower jaw All-on-4?
Risks can include infection, integration issues, prosthesis complications, bite overload, and nerve-related symptoms—one reason CBCT planning is emphasized in the mandible.
Can I eat normally after getting lower jaw All-on-4 implants?
You’ll typically start with softer foods and progress as advised, especially if you have immediate loading. “Normal eating” depends on stability, bite balance, and healing, so your clinic’s instructions matter.
How much does lower jaw All-on-4 cost?
Cost depends on surgical needs , prosthesis materials, and the number of stages or visits required. The safest way to get a real quote is an itemized plan after CBCT.