If you want the most support for a fixed full-arch smile, all on 8 dental implants may be an option, but it isn’t for everyone. More implants can mean more support points, yet it can also mean more planning, more surgical variables, and different cost drivers.
This guide, by Prof Clinic in Istanbul, will help you understand what 8 implants full mouth really means, when All-on-8 is clinically reasonable, how it compares to All-on-4 and All-on-6, and what a realistic journey looks like.
This article is educational and can’t replace an in-person dental exam. A final plan requires a clinical evaluation and 3D imaging (CBCT) to assess bone, bite forces, and gum health.
What are All-on-8 dental implants?
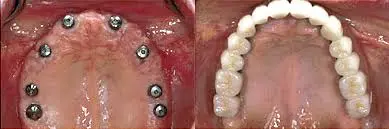
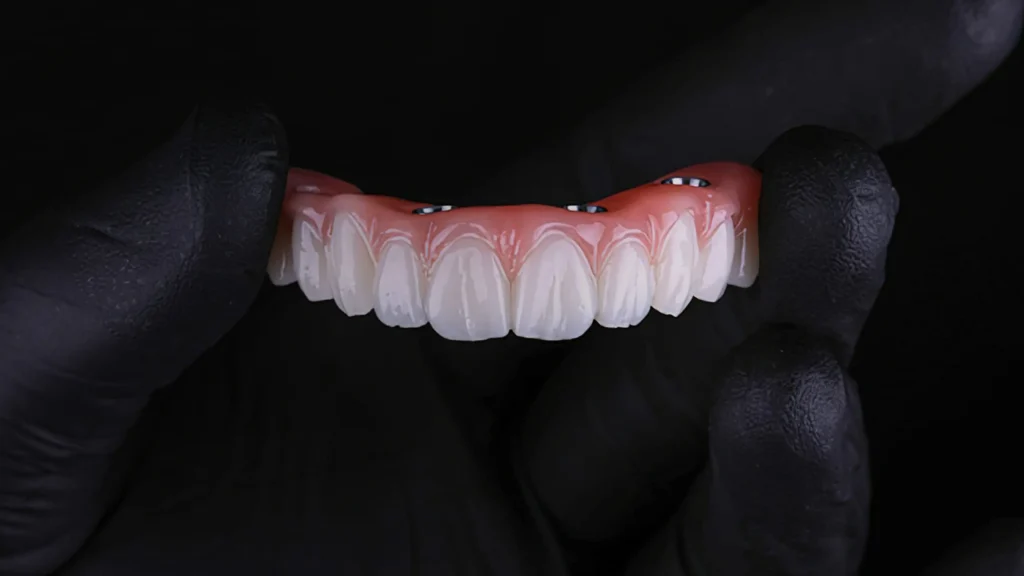
8 implants full mouth describes a full-arch restoration where a fixed bridge is supported by eight implants in a single arch. In everyday search language, people often say full mouth, but clinically it can mean:
- One arch (upper or lower) replaced with an implant-supported full-arch bridge, or
- Both arches treated (upper and lower), which is a bigger plan with more variables.
It helps to think of this as a system: implants, abutments, the bridge, and the way your bite loads that bridge. Implant count is only one part of the design; planning and execution matter just as much.
Many people looking up All-on-8 are:
- Struggling with failing teeth
- Unhappy with removable dentures
- Missing most teeth in one arch and seeking a stable, fixed option
For a broader context on full-arch categories (fixed bridge vs implant-retained denture), our Full Arch Dental Implants guide is a helpful companion.
Why choose All-on-8 dental implants?
When clinicians recommend a maximum implants arch approach, they’re usually trying to solve a specific problem: how to support a full-arch bridge so it handles chewing forces predictably and stays maintainable for the long term.
More implants can provide more support points and may help distribute load in selected cases, but it’s not automatically better for every mouth.
benefits
- More support points for a long span: A full-arch bridge is a long structure; additional implants may help support the span, depending on anatomy and bite forces.
- Planning flexibility: More implants can give the restorative team more options for bridge design and load management if bone quality allows proper placement.
- A maximum support pathway for demanding bites: Patients with higher bite forces or complex bite relationships may be evaluated for designs that increase support, alongside other strategies.
Tradeoffs
- More surgery variables: More implant sites can mean more surgical steps and more emphasis on precise planning and execution.
- More cost drivers: Additional implants can increase component and lab complexity and sometimes chair time, which impacts total cost drivers even when a clinic doesn’t quote per implant.
- Not always needed: Many patients do very well with All-on-4 or All-on-6 when planned appropriately for their bone and bite. At Prof Clinic, we frame full-arch treatment as evaluation-first for this reason.
If your goal is maximum stability, the safest shortcut is a written plan based on CBCT and bite analysis, not a one-size-fits-all implant count, you can start a free online consultation to start that process.
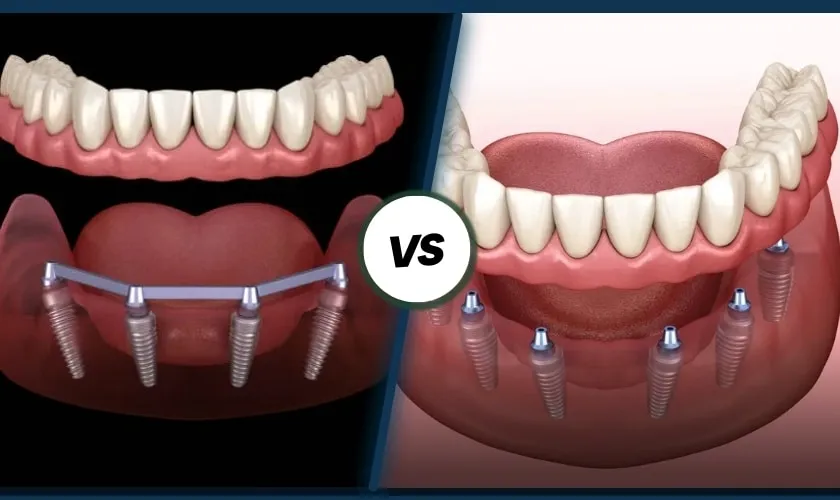
All-on-8 vs All-on-4 vs All-on-6
Here’s the key mindset shift: fewer implants can still be strong when bone, bite, and prosthetic design are appropriate. More implants can be selected when the clinical picture benefits from extra support points.
A good plan chooses the right design for your risk profile, not the biggest number.
All-on-4 vs All-on-6 vs All-on-8
| Option | Implants per arch | Best for | Bone demand | Stability | Temporary teeth same day? | Practical notes |
| All-on-4 | 4 | Many full-arch cases when planned well | Often designed to work around anatomy with strategic placement | Can be highly stable if criteria met | Case-dependent (immediate load depends on stability & bite) | Common full-arch pathway; requires good planning and maintenance |
| All-on-6 | 6 | Patients who may benefit from additional support points | Depends on bone volume or quality | More support points than 4 | Case-dependent | Can be chosen for design flexibility; final choice still imaging-driven |
| All-on-8 | 8 | Maximum support option when justified by anatomy/bite/design goals | Requires adequate bone for safe placement | More support points than 6 (not a guarantee) | Case-dependent | More components and planning; not necessary for everyone; discuss failure/maintenance scenarios upfront |
Some patients don’t actually need a fixed bridge to reach their goals; a removable implant-retained solution may be easier to clean for certain lifestyles or dexterity limitations. A clear comparison can help you decide what you’ll realistically maintain long term. (Prof Clinic Turkey)
If you want background on our All-on-4 approach, see our All-on-4 guide.
Not sure about the difference between All-on-8 vs All-on-4 or All-on-8 vs All-on-6 for your mouth? Book an appointment to discuss a written recommendation with a timeline outline.
Who is a good candidate for All-on-8 implants?
8 implants full mouth can be a fit when your clinical picture supports safe placement and long-term maintenance. The most important candidacy factors are:
1) Bone volume and bone quality
Implant placement requires adequate bone in the planned positions. If bone is insufficient, the team may discuss options like grafting or alternative implant approaches—decided case-by-case after imaging.
2) Gum health and history of periodontal disease
A history of periodontitis and current inflammation can raise future complication risk if not controlled. Peri-implant disease prevention and maintenance planning are not optional in full-arch cases.
3) Smoking status
Smoking is consistently discussed as a risk factor for poorer implant outcomes and peri-implant complications—especially when combined with a history of treated periodontitis. If you smoke, your team will usually recommend cessation (or at minimum, a risk-reduction plan) before and after surgery.
4) Diabetes and general medical stability
Diabetes doesn’t automatically exclude implants, but control matters. Evidence reviews commonly conclude that poorly controlled diabetes is associated with higher complications (including peri-implantitis and implant loss), while controlled diabetes may have more comparable outcomes with proper protocols and maintenance.
5) Bite forces, grinding, and parafunction
If you clench or grind, it doesn’t mean no implants, but it does mean your plan should address occlusion, prosthesis material choice, and protective strategies when indicated.
Are you ready for All-on-8?
- Do I have enough bone for eight safe implant positions in this arch
- What’s my gum health status (active inflammation? history of periodontitis?) and how will it be controlled first?
- Do I smoke and if yes, what’s the clinic’s risk-reduction protocol?
- Is my diabetes (if present) controlled, and who coordinates medical clearance?
- Will I get a written treatment plan that includes temporaries vs final teeth, visit schedule, and maintenance expectations?
- What is the plan B if one implant doesn’t integrate?
- What daily cleaning tools and recall schedule will I realistically follow?
If you want a candid answer, schedule a meeting, so you can submit details and get an initial review.
How does the All-on-8 procedure work?
Exact steps vary, but most maximum implant arch plans follow a structured pathway:
- Consultation and diagnostics
- Dental history, bite evaluation, gum assessment
- 3D imaging and digital planning to map safe implant positions
- Extractions (if needed) and implant placement
- If failing teeth remain, the plan may include extractions at the surgical visit or staged earlier, depending on infection/bone factors.
- Temporary teeth, only if criteria are met
Many patients ask: Can I get temporary teeth the same day?
- Yes, in selected cases. Immediate loading depends on implant stability and bite planning, so not everyone qualifies. At Prof Clinic, we separate implant placement from the decision to load immediately for this reason.
- Healing phase
Implants typically require a healing period for bone integration, and full treatment may involve several months and sometimes multiple procedures.
- Final bridge design and fit
Final teeth are designed for function (bite), hygiene access, speech comfort, and aesthetics. Long-term success is strongly linked to fit and maintainability, not just implant count.
Want clarity on your likely timeline and whether immediate-load is realistic for you? Request a written plan through our dental implant service pathway.
Recovery after All-on-8 implants
Recovery is a phase, not a single day. Your experience depends on surgical complexity, your health, and whether you received temporary teeth immediately.
What recovery commonly feels like
- Early days: swelling, soreness, and fatigue are common after oral surgery; follow prescribed aftercare and hygiene instructions.
- Eating: most people start with soft foods and advance gradually as guided, especially if immediate-load temporaries were placed
- Speech: temporary changes are common; speaking usually adapts with practice and minor adjustments to the prosthesis.
- Return to work: desk-based work may be possible sooner than physically demanding jobs, but your clinician should guide you based on swelling, comfort, and medical factors.
Is maintenance a part of Recovery after All-on-8 implants?
Peri-implant inflammation and peri-implantitis are strongly associated with factors like poor oral hygiene, history of periodontitis, smoking, diabetes, and lack of professional maintenance. Long-term success is built on daily home care plus regular recalls.
What happens if one implant fails in an All-on-8 system?
This is the question many pages skip and it matters. Management is case-specific, but a responsible clinic should discuss likely pathways such as:
- Identify the cause (infection/inflammation, overload, systemic risk factors) and treat it.
- Stabilize the prosthesis (temporary adjustments) while healing is addressed.
- Replace the implant or redesign the prosthesis to function predictably without compromising hygiene access and load control, depending on location and overall support.
Implants are commonly made from materials such as titanium, and full-arch bridges can be fabricated in different prosthetic materials with different wear/weight/repair profiles. Material selection should match bite forces, aesthetics goals, and hygiene needs, and should be explained transparently in your written plan.
Ask your clinic to put the failure plan in writing: what happens if an implant doesn’t integrate, and how follow-ups/maintenance are handled. Schedule your meeting to ask these questions before travel.
Cost factors and how to choose a clinic for All-on-8 in Turkey?
If you’re comparing All-on-8 options, the ethical approach is to focus on cost drivers not generic online price ranges.
What do drive 8 implants full mouth cost?
- Implant number and implant system choice
- Extractions and infection control
- Bone grafting lift needs
- Temporary vs final teeth protocol
- Prosthesis material and lab complexity
- Sedation approach
- Follow-up care, maintenance plan, and complication policy
How to choose a clinic for All-on-8?
Consider these key points:
- Will you receive a written treatment plan based on CBCT + bite analysis?
- Who is responsible for the surgical phase and the prosthetic phase and how do they coordinate?
- What is the clinic’s protocol for dental disease history?
- What determines whether you qualify for same-day temporary teeth?
- How will hygiene be managed under the bridge (tools, recall schedule, cleaning access)?
- What happens if one implant fails—replace, redesign, or staged approach?
- What follow-up support do you get once you return home?
At Prof Clinic Istanbul, we highlight an evaluation-first approach for full-arch decisions and offer free consultation entry points. If you’re considering treatment in Istanbul, start by requesting a written plan and timeline based on your scans.
FAQs about All on 8 Dental Implants
Can temporary teeth be placed on the same day?
Yes, in selected cases. Same-day temporary teeth (immediate load) usually depend on implant stability and bite planning, so not everyone qualifies.
How much do All-on-8 implants cost?
Costs vary widely based on extractions/grafting needs, implant and bridge materials, digital planning complexity, sedation choices, and clinic protocols. The most accurate approach is a written plan after clinical exam and 3D imaging.
Do I need bone grafting before All-on-8 implants?
Not always. Grafting is considered when bone volume/quality is insufficient for stable implant placement; the need is determined after clinical exam and CBCT.
What are the risks or complications of All-on-8 implants?
Possible risks include infection/inflammation around implants, healing issues, and longer-term peri-implant disease—risk is higher with factors like smoking, poor oral hygiene, history of periodontitis, and diabetes (especially if poorly controlled).
Can All-on-8 implants fail, and what happens if one implant fails?
Implant failure can occur in any system. If one fails, clinicians assess the cause (infection/inflammation, overload, systemic risk factors) and may treat the condition, replace the implant, and/or adjust the prosthesis design—management is case-specific.
How long do All-on-8 implants last?
With good planning, hygiene, and regular follow-ups, implants can function for many years; some sources note implants can last a lifetime with proper care, while the bridge may need maintenance over time.
Can All-on-8 be performed with severe bone loss?
Yes. Sometimes, but it must be planned on CBCT. With severe bone loss, a conventional All-on-8 can be harder because it typically needs more available bone. Many patients do better with a CBCT-guided full-arch plan such as All-on-4/All-on-6 with angled implants, grafting, or other advanced anchorage options. The key for “teeth-in-a-day” is whether we can achieve safe primary stability for immediate loading—this is confirmed only on imaging.