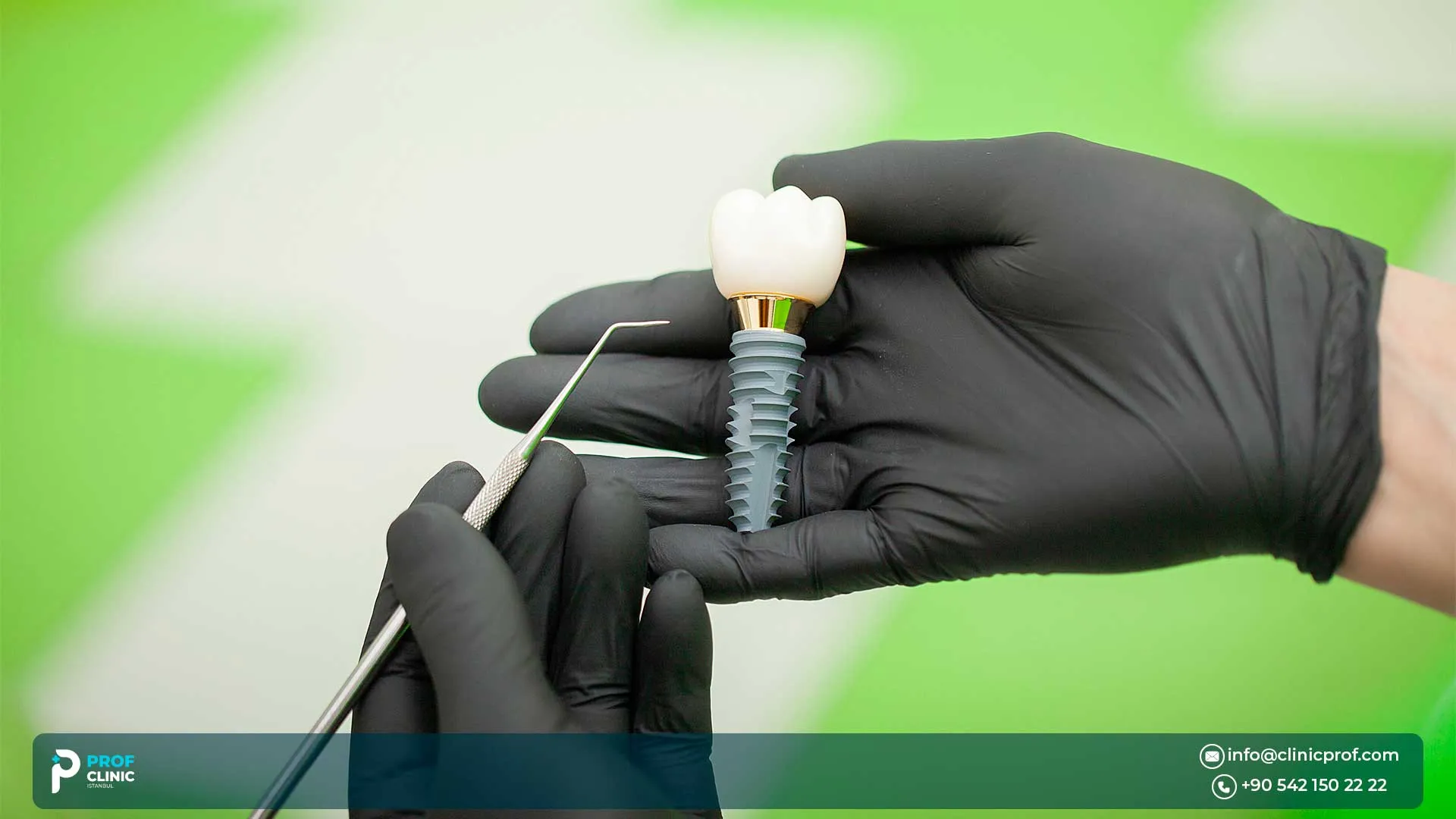
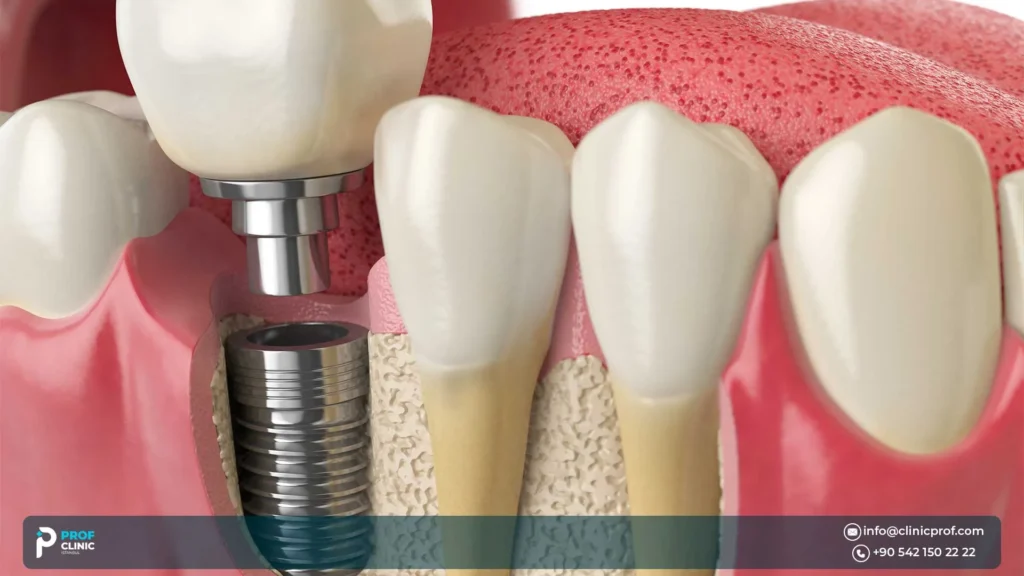
If you’ve been told you have limited space between teeth, or a thin ridge or bone, and you’re wondering whether narrow-diameter dental implants are a safe, proven option, this guide, by Prof Clinic Istanbul, is for you.
The goal is to help you understand what narrow really means, when it’s a smart alternative to grafting, and when a standard implant (or a different plan) is usually safer.
This article is for education only and does not replace an in-person dental exam. Implant suitability depends on your bite, bone volume, medical history, and 3D imaging.
What are narrow-diameter dental implants?
Small diameter implants are dental implants designed for situations where a standard implant may not fit safely, most commonly because of limited interdental space and/or a narrow ridge.
International consensus statements (including the ITI) recognize narrow-diameter dental implants as an appropriate option in selected cases when biomechanics and prosthetic planning are carefully managed, which is why our workflow starts with imaging and a prosthetic-driven plan.
Thin implants are not better implants; they’re more specific implants. When used for the right reasons and with the right prosthetic design, they can avoid or reduce certain augmentation procedures in some cases. When used in the wrong case, such as high forces, poor stability, and unfavorable crown design, they can be more sensitive to complications.
If you want a dentist to evaluate whether narrow is appropriate, start with a planning workflow that includes imaging and a prosthetic-driven plan. At Prof Clinic in Turkey, we describe implant evaluation using radiographic imaging and CT when needed for detail.
What is considered a narrow diameter implant?
Definitions vary slightly by manufacturer and study design, but many widely cited references define the term narrow around ≤ 3.5 mm, and ITI commonly classifies narrow implants into groups by diameter with special caution as you get very small.
To simplify, think about the classification of narrow Diameter Implants in this way:
- Very small (mini): typically < 2.5 mm
- Narrow: 2.5 mm to < 3.3 mm
- Narrow (upper range): 3.3 mm to 3.5 mm
It means that the smaller the diameter, the more sensitive the implant can be to force and prosthetic leverage, especially in posterior teeth.
What is the difference between narrow implants and mini implants?
This is one of the biggest sources of confusion online among our patients and others.
- Mini implants typically refer to extra-narrow diameters, often <2.5–3.0 mm depending on the reference, and are frequently discussed for specific indications, often with one-piece designs in many systems.
- Narrow diameter implants (NDIs) more commonly include two-piece implant systems in the ~2.5–3.5 mm range and are used in selected single-tooth and other indications when space/bone is limited.
Mini and narrow are not interchangeable terms, and the indications and risk profile can differ.

When are narrow-diameter implants indicated?
Small diameter implants are most often considered when you have one or more of these planning problems:
- Limited interdental space: Tight gap between adjacent teeth/roots.
- Thin bone or narrow ridge: Not enough bone width for a standard diameter without augmentation.
- Replacing naturally small teeth: Where prosthetic emergence and spacing are constrained
- Some posterior situations: But only with strong risk control.
If you’re unsure whether you need grafting or a narrow implant, you can request a planning review via WhatsApp through our Dental Implants page or book an appointment.
Can narrow-diameter implants be used in limited interdental space?
Yes. This is one of the core indications, when spacing rules and 3D positioning are respected. The key is that the dentist must protect:
- Adjacent roots: Avoid root damage
- Interproximal bone: Supports gum papilla and long-term tissue health
- A prosthetic emergence profile that can be cleaned and maintained
This is where CBCT and prosthetic-driven planning matter: you’re not just measuring the visible gap—you’re evaluating the root positions and bone envelope in 3D.
Are narrow implants suitable for patients with thin bone?
Sometimes. Thin bone can mean thin width, poor quality, or both.
- If the main issue is width (narrow ridge), an NDI may fit within the available bone in selected cases.
- If the issue is quality (soft bone), achieving stability can be harder, and the plan may shift different implant design, different healing or loading, augmentation, or staged treatment.
In our dental implant evaluation service, we also highlight imaging (X-ray and CT when needed) to understand bone anatomy before deciding the best plan for your case.
Do narrow implants reduce the need for bone grafting?
The thin implants may reduce the need for horizontal augmentation in selected narrow-ridge cases because the implant itself needs less bone width than a standard diameter.
ITI consensus discussions include narrow ridges and limited space as common reasons to consider NDIs.
But important caveats:
- If you’re missing bone height or have sinus-related limitations, grafting may still be needed.
- Sometimes augmentation is recommended anyway to improve long-term soft tissue support and prosthetic contours, especially in the aesthetic zone.
Are narrow implants recommended in the anterior aesthetic zone?
They can be used in the aesthetic zone, but this is often planning-sensitive. The front of the mouth is less forgiving because success is not only the implant survives, but also:
- Gum contour and papilla fill
- Natural emergence profile
- Tissue thickness and long-term stability
- Provisionalization strategy
In some cases, a slightly wider implant plus grafting is chosen for better tissue support. In other cases, a narrow implant is selected to fit safely between roots and preserve bone peaks.
When should narrow implants be avoided?
NDIs are not wrong, but they’re not ideal in every case.
Common risk flags include:
- Heavy bite forces without a mitigation plan
- Unfavorable crown-to-implant ratio: very tall crown acting like a lever
- Inadequate primary stability, especially if immediate or early loading is being considered
- Cantilevers or designs that concentrate lateral forces
- Poor hygiene access or high peri-implant disease risk without a maintenance plan
This is where a frank risk discussion builds trust: sometimes the best plan is a standard implant with augmentation, or a different restorative approach entirely.
Why use narrow implants instead of standard implants?
A balanced way to frame the choice is:
- Standard diameter implants are often preferred when space and bone allow, because they generally offer more forgiving biomechanics (more surface area and often more resistance to overload).
- Narrow implants are chosen when they allow safer placement without compromising adjacent teeth or when they reduce the need for certain horizontal grafting procedures in selected cases.
Systematic reviews evaluating narrow implants report generally high survival in many indications, with outcomes influenced by implant category, indication, and study quality.
The categories below reflect common consensus classifications and how they’re discussed clinically.
| Feature | Standard implants | Narrow diameter implants (NDI) | Mini implants (very narrow) |
| Typical diameter | Often >3.5 mm (varies by system) | Usually ≤3.5 mm | Often <2.5–3.0 mm (term varies) |
| Best-fit situations | Adequate space & bone width | Limited interdental space and/or narrow ridge (selected cases) | More limited indications; often discussed for denture stabilization in some contexts |
| Biomechanical sensitivity | Generally lower | Higher, especially with high forces/posterior) | Often highest; design/indication dependent |
| Prosthetic options | Broad | Broad but often more planning-sensitive | Often more limited / indication-specific |
This second planning mini-table is to clarify the NDI categories commonly referenced in consensus discussions.
| NDI category | Diameter range | Typical planning note |
| Category 1 | <2.5 mm | Often considered mini; caution and indication-specific use |
| Category 2 | 2.5 to <3.3 mm | Useful for limited space/ridge; biomechanics matter |
| Category 3 | 3.3 to 3.5 mm | Often best-documented NDI range for broader indications, including some posterior cases |
What are the advantages and disadvantages of narrow-diameter implants?
Pros
- Fits limited gaps while maintaining safety distances from adjacent roots
- May reduce the need for horizontal augmentation in selected narrow-ridge cases
- Can allow a more prosthetically-driven position when space is the limiting factor (rather than “forcing” a standard implant into a compromised position)
Cons
- Higher sensitivity to overload, especially lateral forces
- In some cases, greater need for splinting or occlusion control
- Less margin for error in positioning (because space is already limited)
Are narrow implants more affordable than standard implants?
It’s not reliable to assume “narrow = cheaper.” Total cost is driven by the whole treatment plan, such as:
- Imaging and diagnostics (CBCT/digital planning)
- Need for grafting (or not)
- Number of implants and complexity of the prosthetic design (single crown vs splinted restorations vs full-arch)
- Temporary restorations and follow-ups
The most useful next step is a personalized plan, not diameter-based price guessing.
If you want a plan that explains alternatives (standard implant, graft vs narrow implant), request an implant assessment through our Dental Implants service page.
Narrow-diameter dental implants: posterior strength and bite forces
The biggest patient question is: “Are narrow implants strong enough?” The honest answer is: often yes in selected cases, but they’re more force-sensitive, especially in the back of the mouth.
Posterior teeth see higher bite forces, and the risk is managed by:
- Choosing the widest feasible diameter for the available bone
- Controlling occlusion (reduce lateral load where possible)
- Using a prosthetic design that reduces bending (e.g., splinting in some cases)
- Identifying and managing parafunction (bruxism)
Are narrow-diameter implants strong enough for posterior teeth?
They can be used in posterior regions in selected situations, especially in the higher NDI range (e.g., around 3.3–3.5 mm) with careful planning.
ITI consensus statements report high mean survival in that range across indications, including posterior, while emphasizing that ranges and outcomes vary by study and follow-up.
Posterior NDIs are not automatically unsafe, but they require more deliberate risk-mitigation than a standard implant in the same position.
How do narrow implants perform under occlusal forces?
A simple way to understand forces:
- Axial forces (straight down) are generally more favorable.
- Lateral forces (sideways) create bending moments and can stress the implant–abutment–crown complex.
Dentists manage this by adjusting the bite, reducing steep contacts, and choosing crown shapes/materials and connector designs that limit overload, especially important for thin implants in posterior sites.
Do narrow implants have a higher fracture risk?
Diameter can be one factor associated with mechanical complications, but fracture risk is multifactorial. The safest takeaway is not “narrow fractures,” but: your plan should minimize overload, especially if you clench/grind or have a long crown.
Can narrow implants be splinted together to increase strength?
Yes. Splinting may be used to distribute forces across multiple implants and reduce stress on any single implant or crown. This is especially relevant when bite forces are high or crown height creates leverage.
Can two narrow implants replace a single mola(r)?
In some situations, two narrow dental implants can be planned to replace one molar to spread load if there is enough mesiodistal space and the prosthetic plan supports it.
This is an approach that can reduce bending stress compared with one implant supporting a wide molar crown—again, highly case-specific.
How does crown-to-implant ratio affect narrow implant prognosis?
Think of a tall crown like a longer lever arm. A higher crown-to-implant ratio can increase bending forces, especially relevant for small-diameter implants.
Dentists manage this by:
- Controlling occlusion (reduce lateral load)
- Using splinting where appropriate
- Adjusting crown contours/contact points
- Considering implant length/position within anatomy limits
How does implant length affect the success of narrow implants?
Length interacts with available anatomy and bone quality:
- More length can increase bone contact area in some cases, but longer isn’t always possible because of sinus or nerves, and isn’t always required.
- The treatment goal is stable anchorage and a prosthetic design that limits overload, not simply longer is better.
Is primary stability harder to achieve with narrow implants?
Primary stability depends on many factors:
- Bone quality (dense vs soft)
- Site preparation technique
- Implant macro-design and surface characteristics
- Positioning within the bone envelope
Diameter can influence stability, but it’s not the only variable. Crucially, stability helps determine whether immediate loading is reasonable.
What torque is recommended when placing narrow implants?
There is no universal torque number that applies to every implant system and every case. Clinicians use manufacturer guidance plus objective stability measures to decide loading protocols.
ITI consensus on loading protocols describes typical stability thresholds used in some protocols (for example, insertion torque in a certain range and/or ISQ targets) for immediate loading, but these are protocol- and case-dependent, not blanket rules.
If you grind/clench or need a back-tooth implant in a tight space, ask for a plan review that includes force assessment and prosthetic design choices. Our Medical Team page is a good starting point to understand who may be involved in your care.
Thin implants: placement, loading, and healing steps
Most narrow implant treatments follow the same overall steps as standard implants:
- Consultation and exam
- Imaging
- Digital/prosthetic planning
- Implant placement
- Healing
- Restoration
- Maintenance
Our implant information highlights the role of imaging (X-ray, and CT when more detail is needed) in planning.
Is the surgical procedure less invasive with narrow implants?
It can be less invasive if a small dental implant avoids grafting, meaning fewer surgical steps overall. But it’s still implant surgery: the implant is placed into bone, and healing is still required.
Can narrow implants be placed using flapless surgery?
Sometimes. Flapless or minimally invasive approaches may be considered when anatomy and planning allow adequate visibility, often relying on careful digital planning and sometimes surgical guidance.
We recommend our blog about Dental Implants Without Surgery: Is It Possible?
Can narrow implants be immediately loaded?
They can be immediately loaded in selected cases, but only when stability and occlusion conditions are favorable. ITI loading protocol consensus statements discuss immediate vs early vs conventional loading and include examples of stability thresholds used in certain documented protocols.
This means that immediate loading is not a default perk of narrow implants; it’s a carefully selected protocol.
What is the healing time for narrow-diameter implants?
Healing time varies based on:
- Bone quality
- Implant location
- Whether loading is immediate/early vs conventional
- Health factors and oral hygiene
Your dentist confirms readiness for the final crown based on clinical stability and healing—not calendar time alone.
If you want a step-by-step plan and timeline tailored to your scan and bite, you can start by booking an appointment
Small diameter implants: crowns, bridges, overdentures
Many narrow implant outcomes are decided by prosthetics as much as surgery.
Good design aims to:
- Keep forces as axial as possible
- Avoid overload and cantilevers
- Create contours that are cleanable and tissue-friendly
Can narrow implants support crowns and bridges?
Often yes, especially for single-tooth restorations in appropriate sites, and for splinted designs when force control is needed. In posterior regions, careful design becomes even more important due to higher forces.
What prosthetic options are available for narrow-diameter implants?
Depending on diameter category, position, and force profile, options may include:
- Single crown, common in suitable spacing.
- Splinted crowns, two adjacent implant crowns connected.
- Small bridges, case-dependent, usually with careful design.
- Overdenture attachments in selected scenarios
Are narrow implants suitable for overdentures?
Overdentures are frequently discussed with very small diameters, but planning is individualized. The key determinants are bone volume, stability, hygiene access, and expected forces. Consensus classifications help differentiate mini and narrow categories, so the indication is clearer.
If you want to explore related restorative options beyond implants, our Dental Treatment hub can help you navigate other services.
Narrow-diameter dental implants: evidence, success rates, risks
Evidence discussions should be honest about definitions:
- Survival typically means the implant is still present and functioning.
- Success often uses stricter criteria (bone levels, absence of certain complications, etc.).
A major systematic review evaluated the success of narrow-diameter implants across indications and categories, emphasizing that outcomes differ by diameter category and context
What is the success rate of narrow-diameter implants?
Across many studies and indications, narrow dental implants show high survival in selected cases, with the important nuance that results depend on:
- Implant category (very narrow vs narrow)
- Indication (anterior vs posterior; limited space; narrow ridge)
- Prosthetic design and force control
- Patient risk factors and maintenance
Systematic reviews and consensus reports generally support NDIs as a valid option when properly indicated, while cautioning that the smallest diameters are more sensitive.
What are the long-term survival rates (5–10 years) of narrow implants?
Longer-term data exist, but not equally for every category and every indication. A retrospective study followed narrow diameter implants over extended follow-up (5–10 years), reporting clinical and radiographic outcomes—useful evidence that long-term function is possible, while still depending on case selection and maintenance.
What complications are associated with narrow-diameter implants?
Complications fall into two broad buckets:
Biological
- Peri-implantitis risk, influenced by hygiene, smoking, systemic health, history of gum disease
- Soft tissue inflammation if contours are not cleanable
Technical
- Screw loosening or component wear
- Crown chipping
- Overload-related issues, especially if bruxism is not managed
The prevention strategy is consistent: good planning, good prosthetics, force control, and a maintenance program.
How do narrow implants perform under parafunctional habits (bruxism)?
Bruxism matters. A recent systematic review reports a higher risk of implant failure in probable bruxers compared with non-bruxers (with an elevated odds ratio in pooled data).
For patients, the actionable takeaways are:
- Tell your dentist if you grind/clench (or have morning jaw fatigue, headaches, or worn teeth).
- Expect discussion of occlusal design, splinting options, and possibly a night guard if recommended.
Are narrow implants a long-term solution?
They can be a long-term solution when the case is well-chosen and the implant is maintained, meaning:
- Risk factors are addressed (especially force and hygiene)
- The prosthetic design is protective
- You commit to professional check-ups and daily home care
If you’d like to see realistic treatment outcomes and set appropriate expectations, our Before & After gallery can be a helpful reference point, paired with a dentist’s evaluation of what’s realistic for your anatomy.
Thin implants: guided surgery and surface considerations
For limited space cases, modern planning is often what makes the difference between possible and predictable.
A common workflow includes:
- CBCT (3D) and clinical exam
- Digital planning (prosthetic-driven positioning)
- Surgical guidance when appropriate, especially when safety distances are tight
Systematic reviews discuss guided implant placement accuracy and how computer-guided workflows can improve placement precision compared with freehand—while still depending on proper case selection and execution.
Are narrow implants compatible with digital guided surgery?
Yes, thin implants are commonly placed with digital planning, and guided surgery can be especially helpful when the risk is positional. The key point is that guided surgery is a tool, not a guarantee—errors can still occur if data capture, guide fit, or execution is poor. (PMC)
What surface treatments improve the success of narrow implants?
Many modern implants use surface modifications intended to support bone response and osseointegration.
Reviews discuss how surface characteristics can influence biological interactions, but outcomes remain dependent on the full clinical context—bone quality, stability, loading, and patient factors.
If you want a narrow-space implant plan built around CBCT and digital planning, start with our Dental Implants page and request a case assessment through a free online consultation.
FAQs about narrow-diameter dental implants
What are narrow-diameter dental implants?
small diameter implants are implants typically used when space or bone width is limited, offering a way to replace missing teeth in selected cases. Suitability depends on an exam and 3D imaging.
When are narrow-diameter implants indicated?
They’re commonly considered for reduced interdental gaps and narrow ridges, sometimes as an alternative to horizontal augmentation, depending on bite forces and prosthetic design.
What is considered a narrow diameter implant?
Many references classify narrow diameter implants as ≤3.5 mm, with sub-categories separating very small “mini” diameters from other narrow ranges.
Are narrow-diameter implants strong enough for posterior teeth?
They can be used in posterior regions in selected situations, especially when forces are managed. Your dentist decides based on risk and anatomy.
Do narrow implants reduce the need for bone grafting?
In some narrow-ridge cases, they may reduce the need for horizontal augmentation, but grafting may still be needed depending on bone volume and site requirements.
What is the difference between narrow implants and mini implants?
Mini often refers to extra-narrow diameters and sometimes one-piece designs, while narrow often includes two-piece systems in slightly larger small diameters; indications and loading differ.
Additional sources
- Implant Placement and Loading Protocols
- The Use of Narrow Diameter Implants in the Molar Area
- Systematic review on success of narrow-diameter dental implants
- Accuracy of implant placement with computer-aided static, dynamic, and robot-assisted surgery: a systematic review and meta-analysis of clinical trials