Choosing the final crown for an implant can feel confusing when you are trying to balance strength, appearance, gumline behavior, and long-term practicality. Many patients are not asking whether a PFM crown dental implant is simply “good” or “bad”; they want to know whether it still makes sense for their case, how it compares with other materials, and whether the trade-offs are worth it.
This guide from Prof Clinic in Istanbul is written for patients considering implant crown treatment in Turkey who want a clearer, case-based answer before deciding on the final restoration. It explains what a PFM implant crown is, how it compares with zirconia and E-max, its main pros and cons, who may be a suitable candidate, what the treatment path looks like, and which questions to ask before choosing the final crown.
This article is educational in purpose. It is designed to help readers compare materials and understand trade-offs before they request a case-specific recommendation.
What Is a PFM Crown Dental Implant?
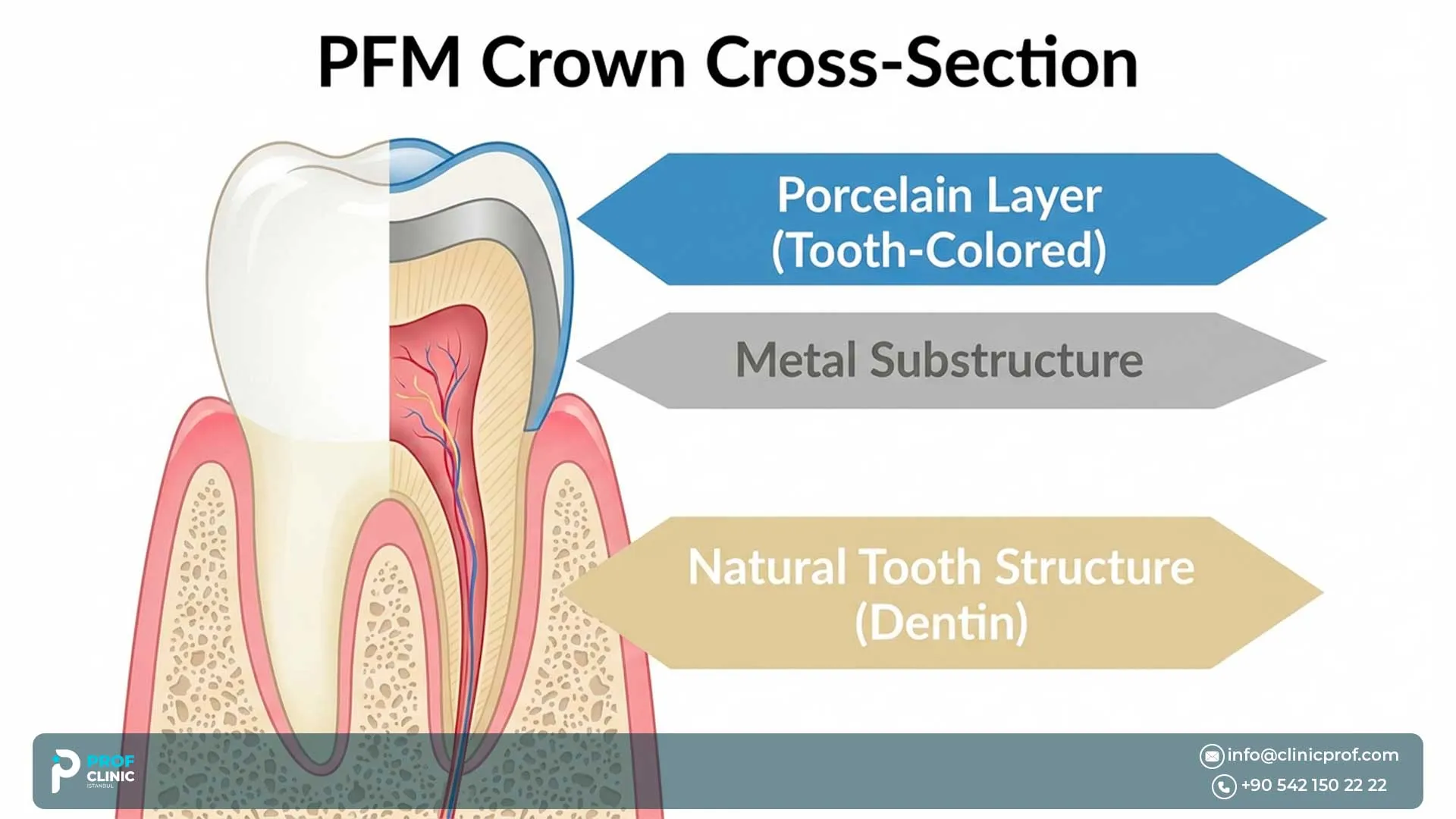
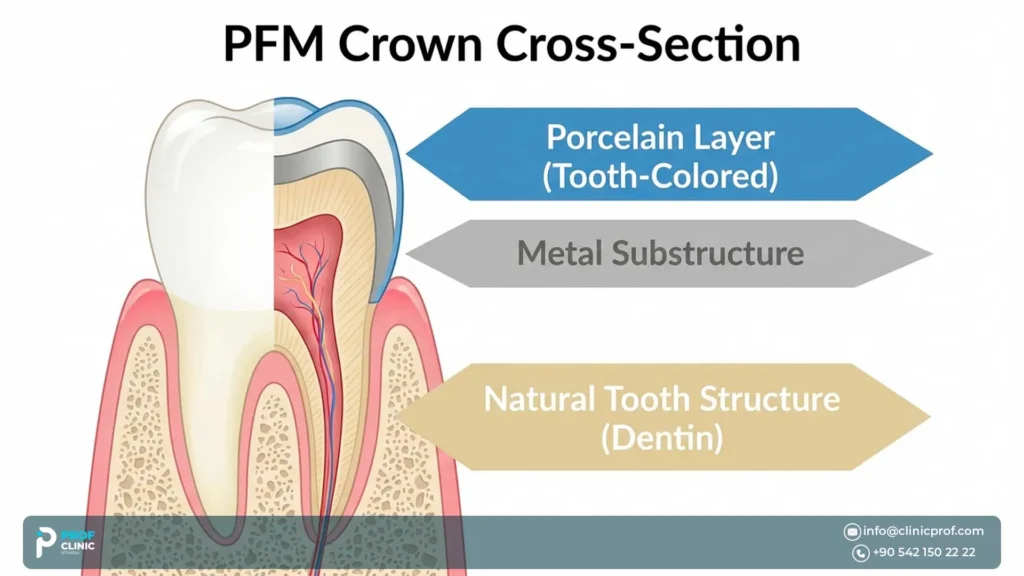
A Porcelain Fused to Metal Crown dental implant is the visible tooth-colored crown placed over an implant restoration. PFM stands for porcelain-fused-to-metal. It combines a metal substructure for support with a porcelain outer layer designed to look more like a natural tooth.
That distinction matters because patients sometimes confuse the crown with the implant itself. The implant is the fixture placed in the jawbone, while the crown is the final visible part attached through restorative components such as the abutment. Our implant page explains the same overall logic: the implant acts as the artificial root, and the crown is the part that restores appearance and chewing function.
PFM is not the only option for implant crowns. Zirconia and other ceramic-based restorations are also widely used, and current evidence does not support treating one material as the universal winner in every case. Crown selection is better understood as a case-dependent decision, not a popularity contest.
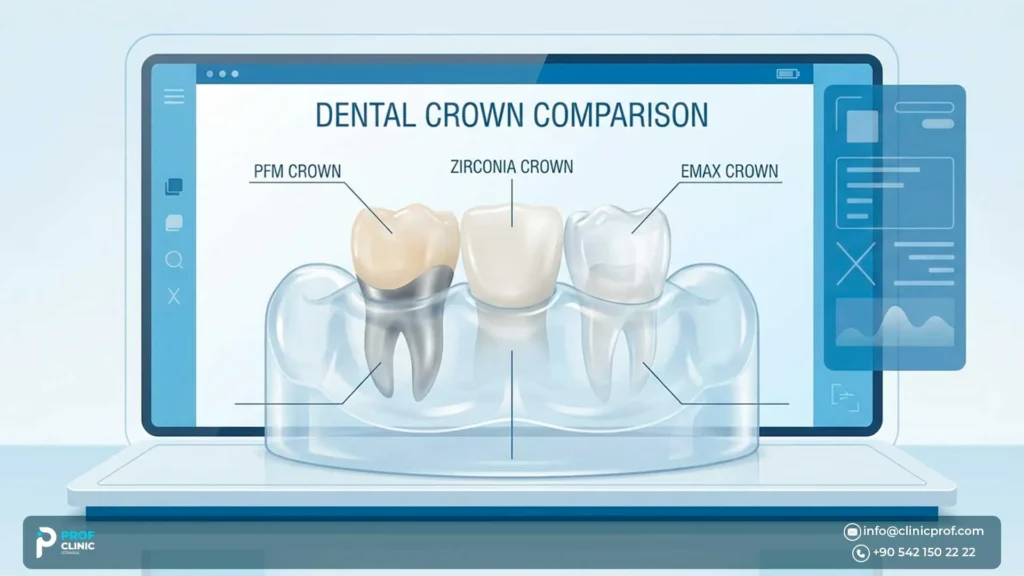
How a PFM Implant Crown Compares With Zirconia and E-max
When patients compare implant crown materials, they are usually balancing four things at once: appearance, bite forces, gumline visibility, and the long-term restorative plan.
A crown that makes sense on a less visible back-tooth implant may not be the first choice in a highly visible smile-zone case. In the same way, a patient with heavy bite forces may not weigh the trade-offs exactly like a patient whose main priority is the most natural translucency possible.
| Material | Strengths | Limitations | Often considered when |
| PFM / metal ceramic crown | Strong, established, practical balance between support and esthetics | Often less translucent; a metal edge may show if gum levels change | Posterior implants, lower smile visibility, or durability-first planning |
| Zirconia implant crown | Metal-free appearance with strong long-term performance in many cases | Design and setup still matter; not every zirconia solution behaves the same way | Patients who want a metal-free look or higher esthetic demand |
| E-max / lithium disilicate crown | Known for translucency and lifelike appearance | Case selection is important, especially on implants or under heavier forces | Carefully selected cases where esthetics lead the discussion |
If you want a deeper look at alternatives after this overview, read our Zirconia Implant Crown and Emax Crowns for Dental Implants blogs that provide additional background.
To get a case-specific opinion after reviewing the trade-offs, you can request a material review through our consultation pathway.
Related guide: Zirconia Implant Crown A Durable and Aesthetic Solution for Your Dental Needs.
Advantages and Disadvantages of PFM Crown on an Implant
Main Pros of a PFM Crown on an Implant
Strong functional support
One of the biggest advantages of a PFM crown is its metal substructure, which gives the restoration solid internal strength. This can be especially useful on implants, where the crown needs to handle daily chewing forces in a stable and reliable way.
Balanced esthetics and durability
The porcelain outer layer helps the crown look more natural than a full-metal restoration, while the metal framework improves strength underneath. For many patients, this creates a good middle-ground solution between appearance and long-term function.
A practical option for back teeth
PFM crowns often make the most sense in posterior areas, where chewing performance matters more than maximum translucency. In less visible parts of the mouth, patients may prefer a restoration that feels dependable and durable over one chosen mainly for high-end esthetics.
Long clinical track record
PFM crowns are well known in restorative dentistry and have been used successfully for many years. That makes them a familiar option for clinicians and a material category with a long history of clinical use rather than a newer approach with less long-term experience.
Valid implant-supported restoration
PFM crowns are not simply “older” restorations that have been replaced by newer materials. Current implant literature still supports metal-ceramic crowns as a valid option, especially when case selection, bite design, and treatment planning are handled properly.
Sensible choice when maximum translucency is not the main goal
In simple terms, a PFM crown can work well when the patient wants a restoration that is functional, proven, and visually acceptable, without making ultra-natural translucency the highest priority.
Main Cons of a PFM Crown Dental Implant
Esthetics are usually weaker than all-ceramic alternatives
The biggest limitation of a PFM crown is usually appearance, especially in highly visible areas. Even when a PFM restoration looks good, it often does not match the light transmission and translucency of more esthetic all-ceramic options such as zirconia-based restorations.
Less ideal for the smile zone
This esthetic limitation becomes more important in front-tooth cases, where even small visual differences can matter to the patient. In the smile zone, patients often care more about lifelike translucency and seamless blending with neighboring teeth, which is where PFM may be at a disadvantage.
Possible dark edge near the gumline
Because a PFM crown contains metal beneath the porcelain, a darker margin can sometimes become visible if the gumline changes or if the soft tissue is thin. This is not guaranteed to happen, but it is an important issue to discuss before treatment, especially in esthetically demanding cases.
Veneer porcelain can chip
Like other layered restorations, PFM crowns can face porcelain chipping over time. This does not mean they are unreliable, but it does mean that crown design, bite forces, and case selection all matter when trying to reduce technical complications.
Material choice should not be treated as “good vs bad”
A common mistake is to assume that one material is simply perfect and the other is outdated. In reality, the discussion is more nuanced: both metal-ceramic and zirconia-based implant crowns can perform well, but the differences often appear in esthetic priorities, veneer behavior, and specific clinical trade-offs.
Possible concern for patients with metal sensitivity
If a patient has a history of metal sensitivity or reactions to dental alloys, this needs to be discussed before choosing a PFM crown. Reported allergic reactions are not the norm, but they are still relevant enough to justify a proper medical and dental history review before final material selection.
For readers who want a trust-focused overview of the professionals involved in treatment planning, see our Medical Team page. If you later decide that you need a case-specific assessment, the clinic also provides an option to book your appointment today.
Who may be a good candidate for a PFM crown implant?
A Porcelain fused to metal crowns implant may be a good fit for patients who want a balanced, practical solution and whose implant is not in the most demanding esthetic position. This often includes posterior single-implant cases, patients with lower smile visibility, or patients who care strongly about function and reasonable esthetics but are not chasing the most translucent ceramic look possible.
It may be less ideal when the implant sits in a very visible front-tooth area and the patient has high esthetic expectations. In those cases, the conversation often shifts toward metal-free options because small differences in translucency and margin behavior become more important. That does not automatically rule PFM out, but it changes the discussion.
Bruxism, clenching, bite pattern, tissue levels, implant position, and restorative design also matter. None of these factors should be reduced to a one-line rule such as “PFM is always better for grinders” or “zirconia is always better in front.” A careful examination is what turns a material choice into a proper treatment recommendation.
Good fit may include
- posterior implant restorations
- lower smile visibility
- patients prioritizing function and practical value
- cases where a balanced strength-esthetics approach makes sense
Less ideal fit may include
- highly visible front-tooth implant cases
- patients seeking the most lifelike translucency possible
- cases where metal margin visibility would be especially undesirable
- situations where the overall restorative plan points clearly toward another material
If you already have an X-ray or written treatment plan and want a later case review, you can use our booking page to request a personalized recommendation and free consultation.

What Does the Treatment Path for a PFM Implant Crown Look Like in Turkey?
Crown material choice should not feel random or last-minute. In a typical implant pathway, treatment starts with examination and imaging, then moves to implant placement, healing, and the restorative stage where the final crown is designed and fitted. At Prof Clinic in Turkey, the dental implant page explains the same broader sequence: diagnosis and imaging first, implant placement next, and restorative components such as abutments and crowns after healing or according to the loading plan.
Some patients also receive a temporary crown before the final restoration. Our temporary-versus-permanent implant crown guide explains that a temporary crown is used during healing, while the permanent crown is the long-term custom restoration. The same page notes that timing varies based on implant stability, implant location, bone and gum condition, and whether grafting or immediate temporization was involved.
A simple way to think about the pathway is this:
- Planning and imaging to assess bone, gums, implant position, and restorative goals.
- Implant placement and early healing.
- Temporary stage in some cases to support healing or appearance while the site matures.
- Final crown design and delivery once the dentist confirms readiness for the definitive restoration.
How to care for a PFM crown dental implant
Long-term success does not depend on crown material alone. A PFM crown dental implant still needs daily plaque control, regular follow-up, and prompt attention if something changes.
The American Dental Association recommends brushing twice daily with fluoride toothpaste and cleaning between teeth daily, while the American Academy of Implant Dentistry advises caring for implant restorations much like natural teeth: brush, floss, and attend regular cleanings and check-ups.
For implant patients specifically, follow-up matters. Guy’s and St Thomas’ NHS guidance notes the importance of regular checks after implant treatment, and our zirconia crown blog also emphasizes follow-up consultations and ongoing oral hygiene for long-term maintenance. Those principles apply to PFM implant crowns as well.
A practical care routine usually includes:
- brushing carefully around the implant restoration every day
- cleaning between teeth or restorations daily
- attending professional reviews and cleaning visits
- reporting looseness, chipping, or a changed bite promptly
- using a night guard if your dentist prescribes one for clenching or grinding
It is better to avoid fixed lifespan promises. Some implant crowns last many years, but hygiene, bite forces, habits, maintenance, and restorative design all affect longevity. Our temporary-versus-permanent guide makes the same point for permanent implant crowns generally: long-term use depends on real-world factors such as grinding, wear, hygiene, and maintenance.

Questions to Ask Before Choosing a PFM Crown Dental Implant in Istanbul
A good consultation is not only about hearing the dentist’s recommendation. It is also about asking the right questions so the answer fits your case rather than a generic crown article.
Ask questions such as:
- Is a PFM crown dental implant suitable for the position of my implant?
- Is my case in a smile zone where translucency matters more?
- Could my gumline make a metal edge more visible over time?
- What are my zirconia or other ceramic alternatives in this case?
- How does my bite or clenching pattern affect the material choice?
- Will I have a temporary crown before the final restoration?
- Is the final recommendation being made for esthetics, function, tissue behavior, or a mix of all three?
These questions help move the conversation from “Which material is popular?” to “Which material fits my anatomy and goals?” That is the point where treatment planning becomes much more useful.
If you want answers based on your own scans or treatment plan, you can book a consultation with us and request a crown-material review before finalizing the restoration.
Choosing the Right Implant Crown Material in Turkey Depends on Your Case
A PFM crown dental implant can be a smart option when durability, practicality, and a balanced appearance matter most. It remains a valid implant-supported restoration rather than an outdated default.
At the same time, it is not ideal for every esthetic situation, and zirconia or other ceramic options may be more attractive in highly visible areas.
The most reliable choice for your case is the one that matches your examination findings, bite, gumline, implant position, and treatment goals.
If you want supporting context before making contact, you can review Medical Team, Before & After, and Testimonials. When you are ready for a case-specific discussion, you can schedule a meeting.

FAQs about PFM Crown Dental Implant
Is a PFM crown a good choice for a dental implant?
It can be. A PFM crown is still a valid implant-supported option when the case needs a balance of strength, function, and acceptable esthetics. The evidence does not support treating it as a universal first choice or as an obsolete material.
Does a porcelain fused metal crown implant look natural?
Usually yes, but it is often less translucent than highly esthetic all-ceramic alternatives. In a visible smile zone, that difference can matter more, and soft-tissue changes may make metal-related margin issues easier to notice in some cases.
Can a metal ceramic crown chip on an implant?
Yes. Veneering porcelain complications can occur with implant-supported restorations, which is why bite, design, and case selection should be discussed before choosing the final material.
Is PFM better than zirconia for implant crowns?
Not in every case. Current evidence supports both as viable options, with trade-offs that tend to involve esthetics, fracture behavior, fit, and the specific restorative setup rather than a simple overall winner.